
Claims Management System (CMS)
For insurers, insurance claims are the moment of truth – when clients have to interact with the company instead of just paying monthly premiums, and actually receive the coverage they have been paying for.
A Claims Management System (CMS) helps insurers organize, track, and speed up the work involved in reviewing, validating, and managing claims. In a market where efficiency, accuracy, and customer satisfaction matter more than ever, the right technology can make the entire claims process far more consistent and manageable.

What is a Claims Management Software? General Definition
Claims management software is a digital solution designed to support insurers in handling claims from first notice of loss through investigation, evaluation, and final settlement.
In simple terms, it gives insurers one central environment to record, review, and manage every stage of a claim instead of relying on disconnected systems, spreadsheets, or manual handoffs.
For insurance companies, the value of claims management software goes well beyond simple efficiency alone.
It helps teams keep all relevant claim information in one place, improves data accuracy, and makes it easier to follow internal procedures and regulatory requirements. When adjusters, case handlers, and other claims professionals work from a shared system, they can make faster decisions based on up to date information rather than incomplete records or email chains.
What’s also important to note is that a modern platform also supports a more structured claims management process by automating repetitive tasks, assigning work to the right people, and creating visibility across the organization. This matters not only for day-to-day operations, but also for broader objectives such as enterprise risk management, fraud control, operational transparency, and better service delivery. In that sense, claims management software is not just an operational tool. It is a business-critical part of how insurers deliver value after a loss occurs.
How Does the Claims Management System Work?
At its core, a CMS guides the claims process from intake to resolution.
It captures incoming claim submissions, routes them through predefined claims workflows, and helps teams assess documentation, communicate with stakeholders, and track progress at every stage. The system creates a structured path for work, which reduces delays and makes the whole process easier to oversee.
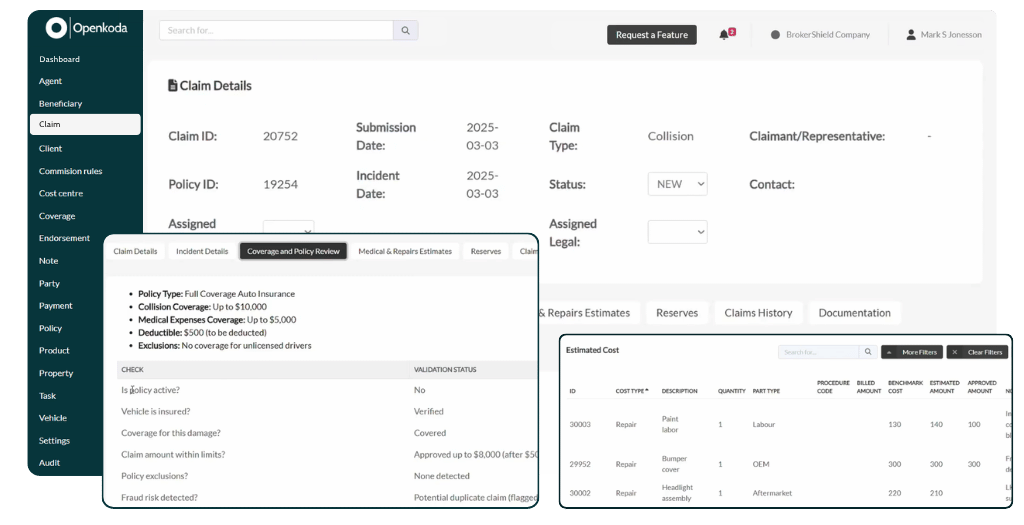
In practice, the system also connects people, rules, and data.
A good CMS allows insurers to review claims data, validate coverage, monitor deadlines, and document decisions in a consistent way. This gives teams stronger control over the claims process, while also helping them gain insights into bottlenecks, fraud indicators, and service performance.
A typical claim flow inside a claims software looks like this:
- Claim intake and registration, with all key claim information entered into the system
- Automatic policy verification and checks against policy administration records
- Assignment of the case to the right adjuster or team based on claim type, severity, or line of business
- Collection of documents, photos, statements, and other supporting evidence
- Review and investigation supported by business rules and internal claims tools
- Ongoing communication with claimants, brokers, partners, or service providers
- Evaluation of loss, reserves, liability, and coverage details
- Approval, rejection, or escalation based on internal rules and authority levels
- Payment processing and final settlement
- Archiving and reporting for audit, analytics, and future reference
[Read also: How to Build a Custom Claims Management Application Faster: Step-by-Step Guide]
Key Features of Insurance Claims Management Software
The best claims management software does more than digitize files.
It improves visibility, speeds up decision-making, and helps insurers build a more reliable claims process across teams and product lines. Below are some of the most important capabilities to look for in claims management solutions:
- Centralized claim handling: A unified workspace makes it easier to manage all claims in one place, reducing duplication and confusion.
- Workflow automation: Automated task routing, reminders, and approvals help streamline claims workflows and reduce manual intervention.
- Document and communication management: Teams can store emails, forms, photos, and notes together, giving everyone access to the same up to date information.
- Rules-based decision support: Built-in logic supports consistent decisions, helps ensure compliance, and reduces errors in the claims process.
- Reporting and analytics: Advanced dashboards help insurers analyze claims data, identify trends, and use data driven insights to improve performance.
- Fraud detection support: Patterns in behavior, suspicious submissions, and anomalies in claims data can be flagged earlier for review.
- Customer and partner communication tools: Better communication supports faster updates and stronger customer satisfaction throughout the claim lifecycle.
- Scalability across products and teams: Good claims management software can support different lines of business, from property and casualty to specialty insurance.
- Audit trails and compliance support: Detailed records of actions, approvals, and changes help insurers ensure compliance and maintain operational transparency.
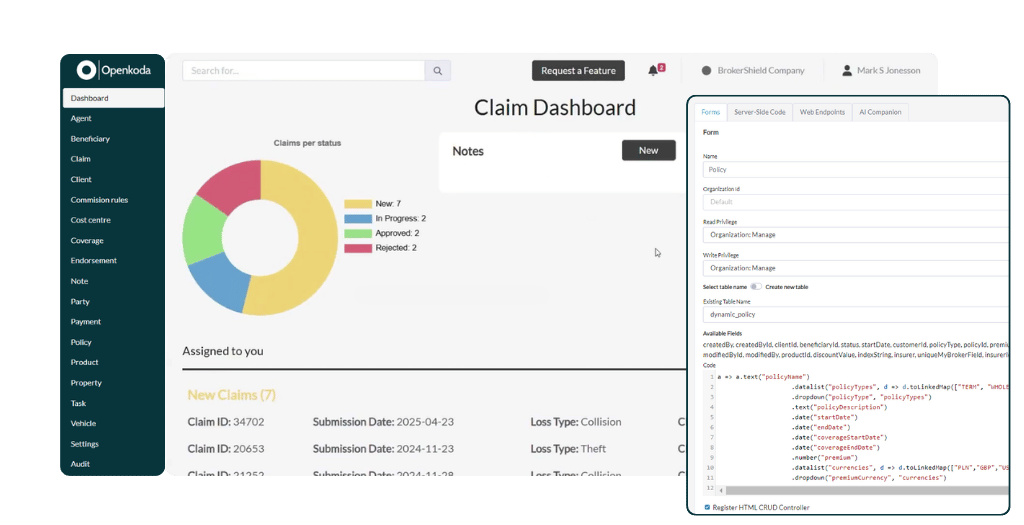
Claims Management System: Key Considerations and Challenges
Even the most capable claims routing software will not deliver strong results if it does not match the insurer’s operational reality. Many organizations still struggle with legacy architecture, fragmented data sources, and manual processes that slow down decision-making. In those environments, introducing a CMS is not only a technology project. It is also a process redesign effort.
One common challenge is balancing standardization with flexibility. Insurers need consistency, but they also need room to adapt flows for different products, regions, regulatory requirements, and claim types. A rigid platform may support simple cases well, yet become a limitation when the business evolves or when more specialized claims professionals need tailored workflows.
Another major issue is visibility. If systems do not share data effectively, users may work with incomplete records, which affects data accuracy, delays decisions, and makes the claims process harder to control. That is why implementation success often depends on governance, clean data structures, and strong process design as much as on software features themselves.
How to Choose the Best Insurance Claims Management Software
hoosing the right claims management software starts with understanding your operational priorities. Some insurers need faster automation for high-volume personal lines claims. Others need a flexible environment for complex specialty cases, partner ecosystems, or multi-step approval paths. The best fit is rarely the one with the longest feature list. It is the platform that supports your business model, your teams, and the way you want to manage future growth.
When comparing options, focus on these three areas:
- Customizability
Insurance operations are rarely one-size-fits-all. The right claims management software should allow you to adapt fields, rules, roles, interfaces, and workflows to your own business logic rather than forcing your teams into a fixed model. - Integration capabilities
Strong integration capabilities are essential because a CMS does not work in isolation. It should connect smoothly with policy administration, billing, document management, analytics, fraud tools, and customer-facing systems. - Reporting and operational insight
A good platform should help insurers gain insights from claims activity, measure performance, and turn operational records into useful intelligence. That is especially important for improving service quality, spotting inefficiencies, and supporting better strategic decisions.
If customizability is your top priority, Openkoda may be a particularly strong option to consider.
Openkoda is a insurtech core platform that helps insurers build tailored internal and customer-facing systems without the limitations of rigid off-the-shelf products, thanks to production-ready application modules including one for claims management.
In practice, that means insurers can create or adapt claims management software around their own processes, products, and user roles. Openkoda supports configurable workflows, broad integration options, and rapid development, which makes it a strong fit for companies that need more than a generic tool. For insurers looking for flexibility, speed, and control, it can be a very practical foundation for building modern claims operations.